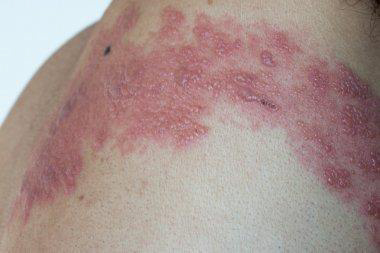
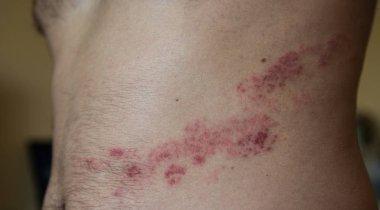
VZV is also called herpesvirus 3 and is a member of the Herpesvirales order of double-stranded DNA viruses.
About 1 million cases of shingles are diagnosed every year in the U.S. The risk of shingles increases as you get older, with about half the cases occurring in people over the age of 50. Shingles develops in about 10% of people who have had chickenpox at an earlier time in their lives.
A person with shingles can pass the varicella-zoster virus to anyone who isn’t immune to chickenpox. This usually occurs through direct contact with the open sores of the shingles rash. Once infected, though, the person will develop chickenpox rather than shingles.
Herpes zoster often affects people with weak immunity. You can get shingles more than one time. One of the biggest myths about shingles is that it can only happen once. This isn’t true. You can have more than one episode. If you get shingles again, you usually don’t get the rash in the same place.
Cause:
After primary infection—varicella—VZV remains dormant in dorsal root ganglia nerve cells in the spine for years before it is reactivated and migrates down sensory nerves to the skin to cause herpes zoster.
It is not clear why herpes zoster affects a particular nerve fiber. Triggering factors are sometimes recognized, such as:
- Pressure on the nerve roots
- Radiotherapy at the level of the affected nerve root
- Spinal surgery
- An infection
- An injury (not necessarily to the spine)
- Contact with someone with varicella or herpes zoster
Clinical features:
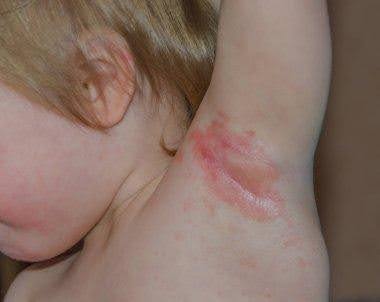
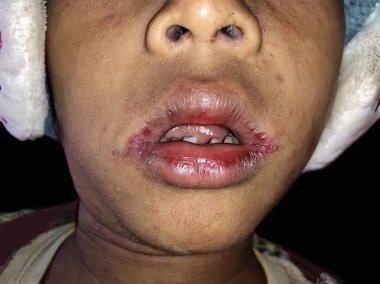
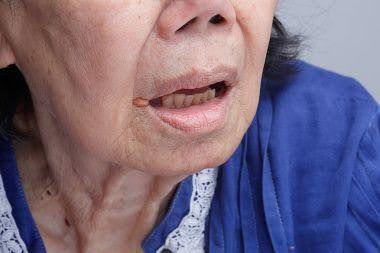
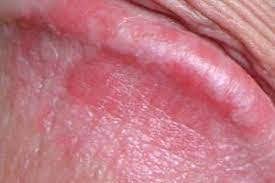
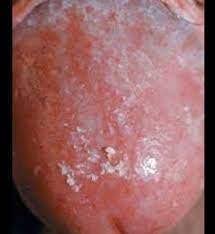
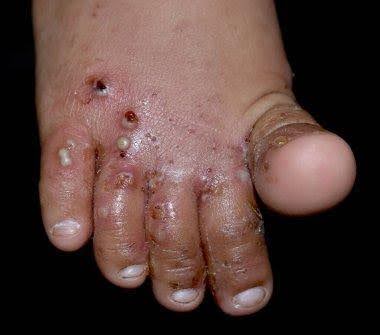
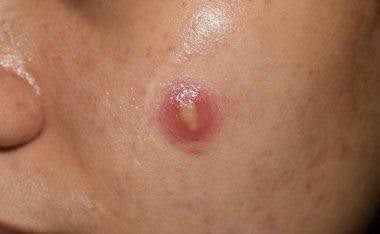
Herpes zoster is characterized by dermatomal distribution, that is the blisters are confined to the cutaneous distribution of one or two adjacent sensory nerves. This is usually unilateral, with a sharp cut-off at the anterior and posterior midlines.
The clinical presentation of herpes zoster depends on the age and health of the patient and which dermatome is affected.
The first sign of herpes zoster is usually localized pain without tenderness or any visible skin change. It may be severe, relating to one or more sensory nerves. The pain may be just in one spot, or it may spread out. The patient may feel quite unwell with fever and headache. The lymph nodes draining the affected area are often enlarged and tender.
Within one to three days of the onset of pain, a blistering rash appears in the painful area of skin. It starts as a crop of red papules. New lesions continue to erupt for several days within the distribution of the affected nerve, each blistering or becoming pustular and then crusting over.
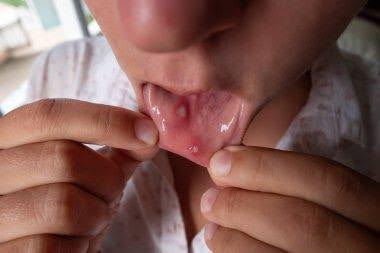
The chest (thoracic), neck (cervical), forehead (ophthalmic) and lumbar/sacral sensory nerve supply regions are most commonly affected at all ages. The frequency of ophthalmic herpes zoster increases with age. Herpes zoster occasionally causes blisters inside the mouth or ears, and can also affect the genital area. Sometimes there is pain without rash.
Pain and general symptoms subside gradually as the eruption disappears. In uncomplicated cases, recovery is complete within 2–3 weeks in children and young adults, and within 3–4 weeks in older patients.
It can take three to five weeks from the time you begin to feel symptoms until the rash totally disappears.
First, a few days before the rash appears, you may feel pain in an area on your skin. The pain is described as itching, burning, stabbing or shooting. This usually happens before the rash comes.
Next, the raised rash appears as a band or a patch, usually on one side of your body. The rash usually appears around your waistline or on one side of your face, neck, or on the trunk (chest/abdomen/back), but not always. It can occur in other areas including your arms and legs.
Within three to four days, the rash develops into red, fluid-filled, painful, open blisters.
Usually, these blisters begin to dry out and crust over within about 10 days.
The scabs clear up about two to three weeks later.
Complications of herpes zoster:
- Involvement of several dermatomes, or sometimes, bilateral eruptions in unique dermatomes
- Eye complications when the ophthalmic division of the fifth cranial nerve is involved
- Deep blisters that take weeks to heal followed by scarring
- Muscle weakness in about one in 20 patients. Facial nerve palsy is the most common result. There is a 50% chance of complete recovery, but some improvement can be expected in nearly all cases
- Infection of internal organs, including the gastrointestinal tract, lungs, and brain (encephalitis)
- Herpes zoster is infectious to people who have not previously had chickenpox.
- Herpes zoster in the early months of pregnancy can harm the fetus, but luckily this is rare. Shingles in late pregnancy can cause chickenpox in the fetus or newborn. Herpes zoster may then develop as an infant.
Post-herpetic neuralgia
Post-herpetic neuralgia is defined as persistence or recurrence of pain in the same area, more than a month after the onset of herpes zoster. It becomes increasingly common with age, affecting about a third of patients over 40. It is particularly likely if there is facial infection. Post-herpetic neuralgia may be a continuous burning sensation with increased sensitivity in the affected areas or spasmodic shooting pain. The overlying skin is often numb or exquisitely sensitive to touch. Sometimes, instead of pain, the neuralgia results in a persistent itch (neuropathic pruritus).
Risk factors include:
Anyone who has ever had chickenpox can develop shingles. Most adults in the United States had chickenpox when they were children. That was before the availability of the routine childhood vaccination that now protects against chickenpox.
- Age: The risk of developing shingles increases with age. Shingles typically occur in people older than 50. And people over the age of 60 are more likely to experience more severe complications.
- Some diseases: Diseases that weaken your immune system, such as HIV/AIDS and cancer, can increase your risk of shingles.
- Cancer treatments: Radiation or chemotherapy can lower your resistance to diseases and may trigger shingles.
- Some medications: Drugs that prevent rejection of transplanted organs can increase your risk of shingles. Long-term use of steroids, such as prednisone, may also increase your risk of developing shingles.
Complications from shingles can include:
- Postherpetic neuralgia: For some people, shingles pain continues long after the blisters have cleared. This condition is known as postherpetic neuralgia. It occurs when damaged nerve fibers send confused and exaggerated messages of pain from your skin to your brain.
- Vision loss: Shingles in or around an eye (ophthalmic shingles) can cause painful eye infections that may result in vision loss.
- Neurological problems: Shingles may cause inflammation of the brain (encephalitis), facial paralysis, or problems with hearing or balance.Skin infections: If shingles blisters aren’t properly treated, bacterial skin infections may develop.
Prevention:
A shingles vaccine may help prevent shingles. People who are eligible should get the Shingrix vaccine, which has been available in the United States since its approval by the Food and Drug Administration in 2017. The Zostavax vaccine is no longer available in the U.S, but other countries may still use it.
Shingrix is approved and recommended for people age 50 and older, whether they’ve had shingles or not. People who’ve had the Zostavax vaccine in the past or don’t know whether they’ve had chickenpox may also receive the Shingrix vaccine.
Shingrix is also recommended for people who are 19 years of age and older who have weakened immune systems due to disease or medication.
Shingrix is a nonliving vaccine made of a virus component. It’s given in two doses, with 2 to 6 months between doses. The most common side effects of the shingles vaccine are redness, pain and swelling at the injection site. Some people also experience fatigue, headache and other side effects. The shingles vaccine doesn’t guarantee that you won’t get shingles. But this vaccine will likely reduce the course and severity of the disease. And it will likely lower your risk of postherpetic neuralgia. Studies suggest that Shingrix offers protection against shingles for more than five years.
Talk to your health care provider about your vaccination options if you:
- Have had an allergic reaction to any component of the shingles vaccine
- Have a weakened immune system due to a condition or medication
- Have had a stem cell transplant
- Are pregnant or trying to become pregnant
- The shingles vaccine is used only as a way to prevent shingles. It’s not intended to treat people who currently have the disease.
There is no cure for shingles but there are treatments for managing the symptoms.
- General measures
- Rest and pain relief
- Protective ointment applied to the rash, such as petroleum jelly.
- Oral antibiotics for secondary infection
Antiviral medications
These drugs may ease the discomfort and make the symptoms stop sooner, particularly if you start them within 72 hours of the first sign of shingles. They may also help prevent the pain that can happen months and years later, called postherpetic neuralgia. These medications include:
- Acyclovir
- Famciclovir
- Valacyclovir
Over-the-counter pain medications may be effective in relieving pain:
- Acetaminophen, Ibuprofen
- Other medications
Antibacterial drugs may be prescribed if you develop a bacterial infection due to the shingles rash. Anti-inflammatory drugs like prednisone may be prescribed if shingles affect your eyes or other parts of your face.
]]>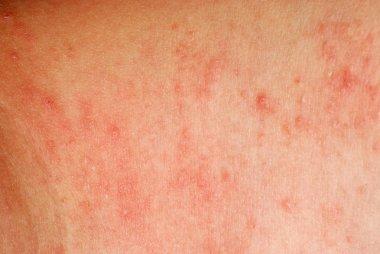
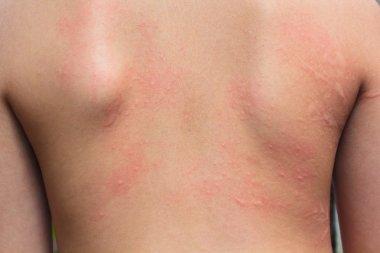
Almost everyone develops at least one skin rash during their lifetime. It’s extremely common to sometimes feel itchy or have red, bumpy skin for a little while.
Infants are prone to diaper rash and cradle cap.
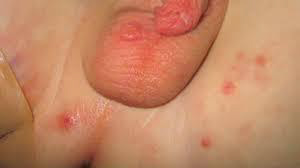
Children are prone to atopic dermatitis and catch rash-inducing viruses, such as fifth disease.
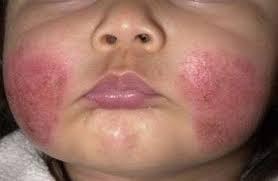
Older kids or adults can develop contact dermatitis as skin becomes sensitive to allergens or irritants over time.

Symptoms of Rashes
The symptoms that come along with a skin rash depend on the cause and type of rash. Some common symptoms include:
- Blistering
- Redness
- Scaly or dry skin
- Similarity to hives
- Blotchiness
- Swelling or inflammation
- Itchy skin
- Pain
- Infection of the areas of broken skin
- Shiny, flat-topped bumps
- Large affected areas of skin
- Circular-shaped affected areas
- Causes of Rashes
Irritants and allergens in the climate/environment can cause rashes on the skin. Other common causes include:
- Viral or bacterial infections
- Skin conditions such as rosacea or eczema
- Stress
- Skin irritants (including soaps, skin care products, or some fabrics)
- Personal and/or family history of allergies, hay fever, or asthma
- Allergic to certain medications, including those that treat high blood pressure, heart disease, and arthritis
- Triggering agents from other conditions, such as hepatitis B or hepatitis C
Some causes and triggers for rashes are unknown.
There are many different types of skin rashes, including:
Contact dermatitis:
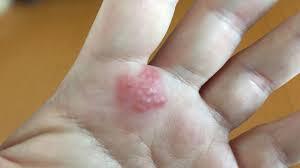
This form of dermatitis occurs when your body reacts to a substance that it doesn’t like. Lots of people are allergic to fragrances, preservatives, nickel (often found in costume jewelry) and poison ivy. Common irritants include soaps, detergents, chemicals and household cleaners.
Eczema:
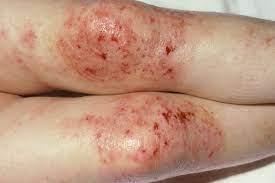
Also called atopic dermatitis, eczema often develops in infancy and often gets better as a child grows. It tends to run in families (genetic). People who have asthma or allergies are more likely to have eczema, too.
Hives:
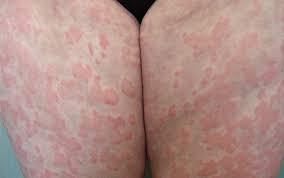
Also called urticaria, hives cause raised, red, itchy skin welts. You may get hives if you have an allergic reaction to airborne allergens or insect stings. Extreme temperature changes and certain bacterial infections can also bring on hives.
Psoriasis:
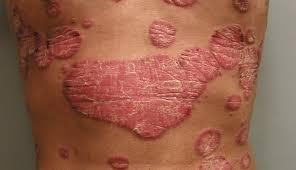
This lifelong skin disorder causes a thick, scaly rash. The rash often forms on the elbows, knees, lower back, scalp and genitals. Psoriasis can be inherited.
Viral: Skin rashes are a common symptom of many viral conditions, such as chickenpox, measles and molluscum contagiosum.
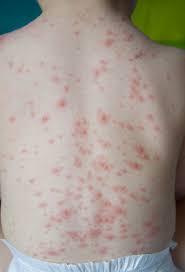
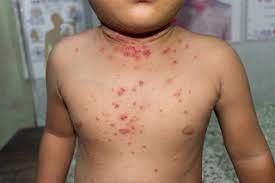
Granuloma annulare
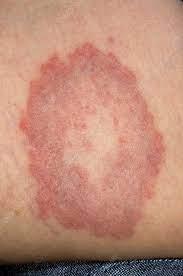
Granuloma annulare is a chronic skin condition. A circular-shaped rash with reddish bumps (papules) is a common symptom. Most often, it affects children and young adults. It’s slightly more common in girls and is usually seen in people who are otherwise healthy. If you have granuloma annulare, you’ll usually notice one or more rings of small, firm bumps over the back of your forearms, hands, or feet. The rash may be mildly itchy.
Lichen planus
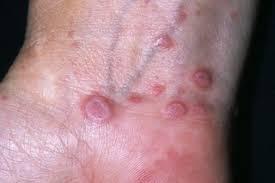
Lichen planus is a common skin condition that causes shiny, flat-topped bumps. They often have an angular shape and a reddish-purplish color. Lichen planus can show up anywhere on the skin but often affects the insides of your wrists and ankles, lower legs, back, and neck. Some people have lichen planus inside their mouth, genital region, scalp, and nails. Thick collections of bumps may occur, especially on the shins.
Pityriasis rosea
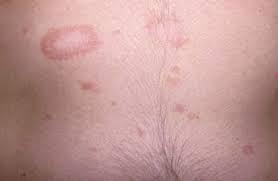
Pityriasis rosea is a common skin rash that is usually mild. The condition often begins with a large, scaly, pink patch of skin on your chest or back. The number and sizes of spots can vary. Pityriasis rosea affects the back, neck, chest, abdomen, upper arms, and legs. The rash can differ from person to person.
Rashes are bothersome and unsightly, but skin rashes usually respond well to treatment. They rarely cause serious problems. Potential issues include:
- Anaphylaxis: A severe allergic reaction can cause a skin rash and a life-threatening condition called anaphylaxis. Extreme swelling (angioedema) from anaphylaxis can close air passages. People in anaphylaxis need an immediate epinephrine injection (EpiPen®) to counteract this allergic response. If you’ve ever felt your throat or mouth swelling when you get a rash, talk to your healthcare provider about whether you need to carry an EpiPen.
- Infection: Scratching an itchy rash can break open the skin, allowing germs to get in. Scratching puts you at risk for developing a bacterial skin infection. Diagnosing a skin rash can be hard because the symptoms can be caused by many things. Your doctor will check your skin and ask about your symptoms and may decide to diagnose your rash using tests such as:
- Skin biopsy: This involves taking a small bit of skin from the affected area and sending it to a lab for testing for a virus or bacteria. (see symptoms and diagnosis of eczema)
- Blood test: Your doctor can diagnose certain diseases by looking at antibodies in your blood. Also, rashes can be the result of systemic conditions, and blood tests can help to check how your organs may be affected.
- Allergy test: These tests include skin pricks or patch tests to look for allergens. During the test, your skin is exposed to certain allergens to detect any potential reactions.
The treatment your doctor recommends will depend on the cause of your skin rash. Some treatment options include:
Over-the-counter and prescription creams and ointments: You can treat rashes caused by skin conditions like eczema with moisturizers that are fragrance-free and contain ingredients such as ceramides, glycerin, and mineral oil. Medications include over-the-counter creams and ointments containing the steroid hydrocortisone (for example, Cortizone-10, Cort-Aid, Dermarest Eczema, Neosporin Eczema). These products may help control the itching, swelling, and redness linked to eczema.
In more severe cases, prescription-strength cortisone creams are also used.
Steroids: If you have ongoing symptoms, your doctor may prescribe topical or oral steroid treatment, which can help with itchy and inflamed skin.
Topical immunomodulators: For people with mild-to-moderate eczema, topical immunomodulators can help. These medications, including brand name products Elidel and Protopic, work by changing the body’s immune response to allergens, thereby preventing flare-ups.
Shots (injections): Injections can be used to treat rashes that come from certain skin conditions. Dupilumab (Dupixent), for example, is an injectable monoclonal antibody used in patients with moderate-to-severe atopic dermatitis. It clears the itch quickly in most patients. Cortisone shots can also be used in more severe cases.
Phototherapy (light therapy): This is another treatment that helps some people with eczema. Phototherapy uses ultraviolet light, either ultraviolet A (UVA) or ultraviolet B (UVB), from special lamps to treat people with severe cases.
Risks linked to phototherapy include burning (usually resembling a mild sunburn), dry skin, itchy skin, freckling, and potential premature aging of the skin. Your health care professionals will work with you to lessen any risks.
Anti-itch products or allergy medications such as antihistamines: Antihistamines, such as Diphenhydramine or Benadryl, can help soothe the itchiness.
Immunosuppressive medications: Medications including steroid shots, prednisone, or other drugs can help clear up a rash by suppressing your immune system.
There are ways to lessen your risk and prevent flare-ups such as those associated with atopic eczema:
- Reduce stress
- Avoid scratchy materials (for example, wool) and chemicals that can be triggers, such as harsh soaps, detergents, and solvents.
- Moisturize often.
- Avoid sudden changes in temperature or humidity.
- Avoid situations that cause sweating and overheating.
- Immediately wash your hands when you come into contact with something you’re allergic to.
Depending on the cause, some skin rashes go away with treatment. Skin conditions like eczema and psoriasis cause chronic, recurring skin rashes that need ongoing care. Treatments can soothe pain, inflammation and itching.
]]>Freckles are the result of an overproduction of melanin. Melanin is a pigment that gives your hair, skin and eyes (your “complexion”) its color.
Freckles on your lips might resemble other lesions, including moles or a lesion associated with Peutz-Jeghers syndrome. This is an inherited condition in which one of the symptoms is dark-colored spots on various parts of your body, including your lips.
Melanin, produced by skin cells called melanocytes, protects your skin from sun damage by absorbing and reflecting ultraviolet light (UV). If you have a light, or fair complexion, your melanocytes make more melanin when your skin is exposed to the sun. Instead of tanning, you’re more likely to develop freckles.
Freckles develop mostly due to exposure to ultraviolet (UV) radiation from the sun. Other causes include:
- Genetics: Several genes are associated with freckling.
- Xeroderma pigmentosum: This is a rare disease that causes increased sensitivity to ultraviolet light, such as the sun.
There are two categories of freckles: ephelides and solar lentigines. Ephelides are the common type most people think of as freckles. Solar lentigines are dark patches of skin that develop during adulthood. This includes freckles, aging spots, and sunspots. The two types of freckles can look similar but differ in other ways such as their development.
Ephelides:
Ephelides are flat and usually red or tan-to-brown in color. Ephelides are the freckles that most people think of when they hear the word “freckle.” Sun exposure and sunburns mainly cause them. They typically appear on body areas exposed to the sun: face, arms, upper chest, neck and back. People with lighter hair color and skin color are more prone to ephelides. They’re mainly seen on people who are white and people of Asian descent. Ephelides tend to first appear in young children who are exposed to the sun. Ephelides continue to develop into young adulthood. Ephelides tend to fade with age.
Solar lentigines:
Solar lentigines are yellow to red to brown to dark patches of skin. They’re also called actinic lentigines, liver spots or age spots, as they usually develop in adults over age 40. Repeated sun exposure over time mostly causes them, and they’re found on exposed areas of skin, including your face, forearms, back of your hands, chest, back, shoulders and lower legs.
The differences between ephelides and solar lentigines are summarized in this table:
| Identifiers | Ephelides | Solar lentigines |
| Origin | sun exposure and genetic makeup | primarily result of sun exposure |
| Appearance | first visible at 2 to 3 years of age after sun exposure and fade with age | accumulate with age, especially after the age of 40, unlikely to fade |
| Areas affected | appear on the face, neck, chest, and arms | most common in sun-exposed skin, face, hands, forearms, chest, back, and shins |
| Sun exposure | appear mostly in the summer, fade during winter | do not change with the season |
| Size | 1 to 2 millimeters, though they can be larger | 2 millimeters or larger |
| Border (edge of skin lesion) | irregular and well-defined | commonly well-defined |
| Color | red to light brown | light yellow to dark brown |
| Most frequent location | Face, arms, neck, chest. | Face, back of hands, chest, forearms, back, shoulders, shins. |
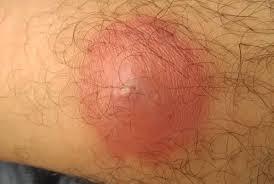
boil
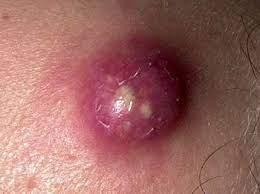
carbuncle
Cause:
Boils are usually caused by the bacteria Staphylococcus aureus (staph infection), but other bacteria and fungi can cause them too. Bacteria enter your skin through a cut or a hair follicle (the opening in your skin where hair grows out). Your body’s immune system responds by sending infection-fighting white blood cells to the area. The white blood cells build up, along with damaged skin, to form pus.
Most people with boils are otherwise healthy and have good personal hygiene. They do however carry Staphylococcus aureus on the surface of their skin (staphylococcal carrier state). Why this occurs is usually not known, but it is estimated that 10–20% of the population are staphylococcal carriers. Staphylococcus aureus is most commonly carried in the nostrils, armpits, between the legs and in the cleft between the buttocks. It may be transferred to other sites from the nostrils via the fingernails.
Tiny nicks or grazes or something rubbing against the skin can inoculate the bacteria into the wall of a hair follicle which is a weak point in the skin’s defense. Once inoculated, the bacteria cause a boil which goes on to run its usual course of about 10 days.
Boils vs. pimples. Pimples are caused by clogged pores, but boils stem from an infection. That’s why you might notice boils around scratches or cuts, unlike pimples. Pimples aren’t contagious, but boils can be. A boil will likely grow faster than a pimple and hurt more and it won’t get better when you use pimple treatments.
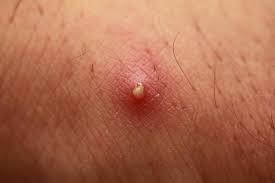
Pimple
Boils vs. cysts. A cyst isn’t caused by an infection. It doesn’t hurt and is usually harmless. Cysts usually grow more slowly than boils. Fluid might come out if you squeeze a cyst, but it’s not whitish-yellow pus, which is a sign of infection. Cysts aren’t contagious, but you can spread boils to others.
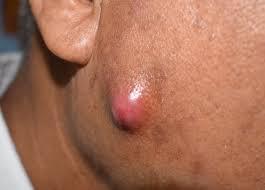
cyst
Common Boil Locations
Boils in the groin area: Boils can affect the skin folds of the groin, the pubic area, and the lips and folds of the vagina. This area has lots of hair follicles and can be prone to chafing, especially if you wear tight-fitting clothes. You can also develop a boil after you get a cut or ingrown hair due to shaving this area.
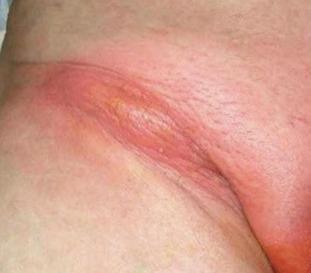
Boils on buttocks: Boils frequently affect the buttocks due to hair follicles, sweat, and friction in the area. Dirty underwear could make a boil here more likely.
Boils on the face: Boils on your face are different from cysts and pimples, though they can look similar. Cysts are filled with fluid, while a pimple is the result of a clogged pore. Cysts and pimples aren’t contagious like boils can be.
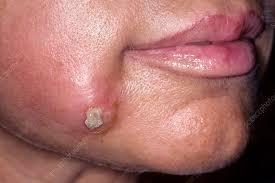
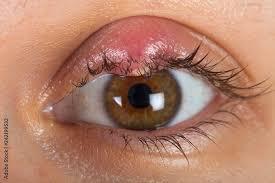
Boil on eyelid: If a boil occurs here, it’s called a stye, and it can be painful. You treat them similarly to the way you treat a boil anywhere else. If it doesn’t go away on its own, a dermatologist can prescribe an antibiotic cream or eye drops.
Other areas where boils often appear include:
Breasts, Armpits, Shoulders, Legs
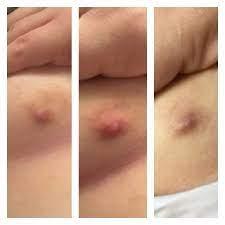
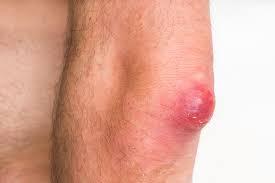
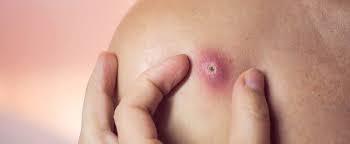
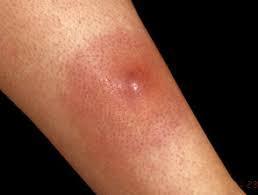
Signs and symptoms of a boil usually include:
- A painful, red bump that starts out small and can enlarge to more than 2 inches (5 centimeters)
- Reddish or purplish, swollen skin around the bump
- An increase in the size of the bump over a few days as it fills with pus
- Development of a yellow-white tip that eventually ruptures and allows the pus to drain out
Risk factors
Although anyone — including otherwise healthy people — can develop boils or carbuncles, the following factors can increase your risk:
Close contact with a person who has a staph infection. You’re more likely to develop an infection if you live with someone who has a boil or carbuncle.
Diabetes: This disease can make it more difficult for your body to fight infection, including bacterial infections of your skin.
Other skin conditions: Because they damage your skin’s protective barrier, skin problems, such as acne and eczema, make you more susceptible to boils and carbuncles.
Compromised immunity: If your immune system is weakened for any reason, you’re more susceptible to boils and carbuncles.
Complications:
Rarely, bacteria from a boil or carbuncle can enter your bloodstream and travel to other parts of your body. The spreading infection, commonly known as blood poisoning (sepsis), can lead to infections deep within your body, such as your heart (endocarditis) and bone (osteomyelitis).
Prevention
It’s not always possible to prevent boils, especially if you have a weakened immune system. But the following measures may help you avoid staph infections:
- Wash your hands regularly with mild soap. Or use an alcohol-based hand rub often. Careful hand-washing is your best defense against germs.
- Keep wounds covered. Keep cuts and abrasions clean and covered with sterile, dry bandages until they heal.
- Follow a balanced healthy diet with meat, plenty of fruit and vegetables.
- Avoid smoking.
- Change your underclothes and night attire regularly.
- Consider modifying leisure activities that cause sweating and friction from clothing, such as squash and jogging.
- If you are iron deficient, a course of iron tablets may help reduce infection.
- 1000 mg of vitamin C each day has also been advocated to improve deficient neutrophil function.
- Avoid sharing personal items. Don’t share towels, sheets, razors, clothing, athletic equipment and other personal items. Staph infections can spread via objects, as well as from person to person. If you have a cut or sore, wash your towels and linens using detergent and hot water with added bleach, and dry them in a hot dryer.
Treatment of boils depends on their severity:
Apply warm compresses: Soak a washcloth in warm water and then press it gently against the boil for about 10 minutes. You can repeat this a few times throughout the day. Once you see the pus at the center (that’s called “bringing a boil to a head,” it’ll probably burst and drain soon. This usually occurs within 10 days after you see the head.
Use a heating pad: A heating pad can help the boil start to drain, too. Put the heating pad over a damp towel and lay it on the affected area. It may take up to a week for the boil to start opening and draining the pus. Keep applying heat, either with a heating pad or compress, for up to 3 days after the boil opens.
Antiseptic or antibacterial soap in your daily bath or shower for a week then twice weekly for several weeks. The cleanser may cause a little dryness.
Use a hand sanitizer regularly to reduce the chance of reinfecting yourself or others with contaminated hands.
Antiseptic or antibiotic ointment or gel to apply to the inside of the nostrils.
Wipe the entire skin surface daily for a week with 70% isopropyl alcohol in water (this will make the skin dry).
Apply a topical antiseptic such as povidone iodine or chlorhexidine cream to the boils and cover with a square of gauze.
Your doctor may prescribe an oral antibiotic (usually the penicillin antibiotic flucloxacillin), sometimes for several weeks.
Other members of the family with boils should also follow a skin cleansing regime. Your doctor may also advise the family to apply topical antibiotics to their nostrils in case they are Staphylococcus aureus carriers as well.
If the boils fail to clear up, a swab should be taken for microbiological culture, in case of methicillin (meticillin) resistant staphylococci.
Sometimes, special antibiotics may be prescribed on the recommendation of a specialist, including fusidic acid, clindamycin, rifampicin and cephalosporins.
Most boils will disappear on their own or with simple home treatment. In rare cases, the bacteria can enter your bloodstream and affect other parts of your body which could lead to more serious infections.
]]>Birthmarks are very common but not everyone has one. An estimated 10% of all babies born around the world have a specific birthmark called a hemangioma.
Birthmarks may be caused by extra pigment-producing cells in the skin or by blood vessels that do not grow normally. Most birthmarks are painless and harmless. In rare cases, they can cause complications or are associated with other conditions.
CAUSE:
The exact cause of why birthmarks develop is unknown. In some cases, birthmarks form because:
- Blood vessels don’t form as expected during fetal development (vascular birthmarks).
- Melanocyte cells (the cells that give your skin color) grow in clusters (pigmented birthmarks).
- A type of birthmark runs in your biological family history (genetic predisposition).
- An underlying medical condition causes birthmark development (nevus sebaceous syndrome, skin cancer or neurofibromatosis).
There are two main categories of birthmarks — vascular birthmarks and pigmented birthmarks:
Vascular birthmarks:
These birthmarks are made of blood vessels that didn’t form as expected during fetal development. This type of birthmark is also known as a red birthmark. Color from the birthmark comes from blood vessels in your skin. These may be present at birth or develop shortly after birth.
Vascular birthmarks include:
Strawberry hemangiomas (strawberry birthmark, nevus vascularis, capillary hemangioma, hemangioma simplex) might appear anywhere on your body, but are most common on your face, scalp, back or chest. They consist of small, closely packed blood vessels. They might be absent at birth and develop after several weeks. They usually grow rapidly, remain a fixed size and then fade. In most cases, strawberry hemangiomas disappear by the time a child is 9 years old. Some slight discoloration or puckering of the skin might remain at the site of the hemangioma.
Cavernous hemangiomas
Cavernous hemangiomas (angioma cavernosum, cavernoma) are similar to strawberry hemangiomas but extend deeper below the surface of your skin. They might appear as a red to blue spongey mass of tissue filled with blood. Some of these lesions disappear on their own, usually as your child approaches school age.
Port-wine stain birthmarks
Port-wine stain birthmarks are flat, purple-to-red birthmarks made of dilated blood capillaries. These birthmarks occur most often on your face and might vary in size. Port-wine stains are permanent (unless treated) and might thicken or darken over time. These may cause self-esteem concerns if they’re in a prominent area of your body.
Salmon patches
Salmon patches (stork bite or angel kiss birthmarks) appear on 30% to 50% of newborn babies in the U.S. These marks are small blood vessels (capillaries) that are visible through your child’s skin. They’re most common on their forehead, eyelids, upper lip, between the eyebrows and the back of their neck. These marks fade as your child grows.
Pigmented birthmarks:
Pigmented birthmarks are made up of a cluster of melanocyte cells (the cells that give your skin color). These birthmarks have a color that’s different from the color of the rest of your skin. Pigmented birthmarks might range from brown or black to bluish.
Pigmented birthmarks include:
- Dermal melanocytosis (formerly called Mongolian spots) are usually bluish and look like bruises. They often appear on the buttocks and/or lower back, but they sometimes appear on your trunk or arms.
- Pigmented nevi (moles) are raised growths on your skin that are the same color as your natural skin tone, or brown or black. Moles can appear anywhere on your skin, alone or in groups.
Congenital nevi
Congenital nevi are moles that are present at birth. About 1 in 100 people are born with one or more moles. These birthmarks have a slightly increased risk of becoming skin cancer, depending on their size. Larger congenital nevi (more than 20 centimeters) have a greater risk of developing into skin cancer than smaller congenital nevi. All congenital nevi should be examined by a healthcare provider, along with any changes to these birthmarks.
Café-au-lait spots
Café-au-lait spots are light tan or light brown spots that are usually oval in shape. They appear at birth but might develop in the first few years of a child’s life. One café-au-lait spot isn’t cause for concern, but multiple spots larger than a quarter may be a sign of an underlying condition called neurofibromatosis.
Birthmarks look different on each person and vary in size, shape and color. Features of a birthmark include:
- A flat or raised mark on your skin.
- The mark is the size of a pinhead to the size of your fist.
- The color of the mark is different from the skin around it (pink, red, purple, tan, brown or black).
- Pigmented birthmarks might increase in size as you age and change colors, especially after sun exposure and during times of hormone changes. They can become itchy and might occasionally bleed when injured.
Complications:
Complications of pigmented birthmarks can include psychological effects when the birthmark is located in a prominent area of your body, like on your face. This can affect your self-esteem and how you feel about your appearance.
Pigmented birthmarks also can pose an increased risk of skin cancer. A healthcare provider should check any changes that occur in the color, size or texture of a mole. See a provider right away if you have any pain, bleeding, itching or swelling of a birthmark.
Diagnosis :
A healthcare provider can diagnose a birthmark after a physical exam to get a closer look at the mark on your skin. If your birthmark is deep within your skin, a provider can confirm it with an imaging test like an MRI (magnetic resonance imaging), ultrasound or CT (computed tomography) scan. A skin biopsy might be necessary if you have a birthmark that changes in size or shape and may be a sign of skin cancer.
Prevention
There’s no way to prevent the development of birthmarks. You can reduce your risk of birthmarks changing color or developing into skin cancer from sunlight exposure by protecting your skin from the sun’s ultraviolet rays. Wear sunscreen and protective clothing when you’re outside to reduce your risk. You can also avoid sun exposure during the daytime when the sun is at its brightest, between 10 a.m. and 4 p.m.
Treatment to remove a birthmark may include:
- Cryotherapy.
- Laser removal.
- Surgical removal.
- Injections of cortisone.
A healthcare provider can review your birthmark and let you know what your best treatment options would be. Providers usually treat childhood birthmarks after a child reaches 6 years old. They might treat them earlier if they affect the function of your child’s organs, like their vision or breathing.
You may be at risk of scarring if you have a birthmark surgically removed. Surgeons take extra precautions during procedures to reduce your risk of scarring. You may also be at risk of developing an infection after a removal procedure. To avoid these risks, talk to your surgeon or provider about how you can take care of your skin as it heals after treatment.
]]>
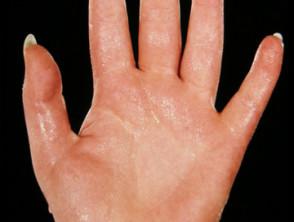
Sweat is an odorless fluid released from your eccrine glands (sweat glands). Sweat’s job is to help regulate your body temperature and prevent overheating. You have eccrine glands in your skin. Sweat moves from your glands through tubes called ducts until it reaches the surface of your skin. Once sweat leaves the ducts, it changes from a liquid to a gas and disappears from your skin (evaporates) to cool down your body.
Hyperhidrosis is common. Research suggests that an estimated 3% of adults in the United States between ages 20 and 60 have hyperhidrosis.
Sweat comes from eccrine glands, which exist in the skin throughout your body. You have the most eccrine glands in your:
Armpits or underarms (axillary hyperhidrosis).

Soles of your feet (plantar hyperhidrosis)
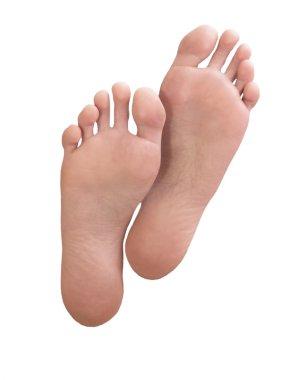
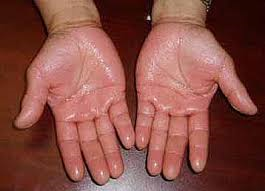
Palms of your hands (palmar hyperhidrosis).
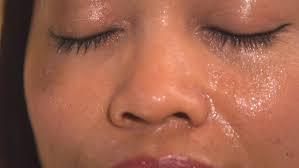
Forehead and cheeks (craniofacial hyperhidrosis).
Genitals.
Lower back.
The most common location on your body to experience excessive sweating is the palms of your hands.
Cause:
Overactive sweat glands cause hyperhidrosis. Your eccrine glands (sweat glands) create sweat to cool down your body when you get hot. This process activates when you exercise or if you’re nervous. If you have hyperhidrosis, your eccrine glands activate and produce sweat more often than when your body is too hot. You may experience sweating at random times of the day when there isn’t something like an activity or emotion causing your glands to produce sweat. Research is ongoing to learn more about why your glands make too much sweat.
There are two types of hyperhidrosis:
Primary focal hyperhidrosis: Focal hyperhidrosis is a chronic skin condition. A genetic change (mutation) causes this condition. You can inherit it from your biological family. This is the most common type of hyperhidrosis. It usually affects your armpits, hands, feet and face. It tends to start before age 25.
Secondary generalized hyperhidrosis: Generalized hyperhidrosis is excessive sweating caused by an underlying medical condition or it’s a side effect of a medication. Some examples include diabetes and Parkinson’s disease and medications, such as naproxen (Aleve®). Generalized hyperhidrosis may cause you to sweat while sleeping.
Triggers that cause sweating:
- Certain emotions like stress, anxiety, fear or nervousness.
- Warm temperatures or humidity.
- Exercise or physical activity.
- Wetness on your skin.
- Damp clothing.
- Beads of fluid dripping from your cheeks or forehead.
- Certain foods and beverages, like spicy foods, fatty foods, sugary and salty foods, and foods with high levels of protein. Beverage examples include caffeinated beverages (coffee) and alcohol.
Over time, hyperhidrosis can lead to the following symptoms:
- Itching and inflammation when sweat irritates your skin.
- Body odor, which occurs when bacteria on your skin mixes with sweat particles.
- Cracked or peeling skin on your feet.
- Hyperhidrosis symptoms can range in severity. You may have minor symptoms that come and go or you may have constant symptoms that have an impact on your day-to-day activities.
- Medications that cause sweating
Certain medications can cause sweating as a side effect, including but not limited to:
- Albuterol (Proventil®).
- Bupropion (Wellbutrin®).
- Hydrocodone.
- Insulin (Humulin® R, Novolin® R).
- Levothyroxine.
- Lisinopril.
- Naproxen (Aleve®).
- Omeprazole (Prilosec®).
- Sertraline (Zoloft®).
Hyperhidrosis (generalized) could be a sign of an underlying medical condition including but not limited to:
- Acromegaly.
- An infection (tuberculosis).
- Anxiety.
- Cancer.
- Diabetes.
- Heart disease or heart failure.
- Hyperthyroidism.
- Menopause.
- Obesity.
- Parkinson’s disease.
You may be more at risk of hyperhidrosis, specifically focal hyperhidrosis, if someone in your biological family has the condition. Research indicates that a hereditary genetic mutation or change to your DNA could cause hyperhidrosis.
Hyperhidrosis can cause complications that include:
- A skin infection.
- Skin changes, such as paleness, discoloration, cracks or wrinkles.
- Maceration, or unusually soft, moist skin.
Hyperhidrosis can also impact your mental health. You may find yourself changing your routine to hide your symptoms from others. Constant sweating may be so severe that you avoid common actions, such as lifting your arms or shaking hands. You may even give up activities you enjoy to avoid problems or embarrassment from excessive sweating. Contact a healthcare provider if hyperhidrosis affects your mental health and social well-being.
Hyperhidrosis is usually diagnosed clinically. Tests relate to the potential underlying cause of hyperhidrosis and are rarely necessary for primary hyperhidrosis.
- The precise site of localized hyperhidrosis can be revealed using the Minor test.
- Iodine (orange) is painted onto the skin and air-dried.
- Starch (white) is dusted on the iodine.
- Sweating is revealed by a change to dark blue/black color.
- Screening tests in secondary generalized hyperhidrosis depend on other clinical features but should include as a minimum:
- Blood sugar / glycosylated hemoglobin
- Thyroid function
Treatment:
- General measures
- Wear loose-fitting, stain-resistant, sweat-proof garments.
- Change clothing and footwear when damp.
- Socks containing silver or copper reduce infection and odor.
- Use absorbent insoles in shoes and replace them frequently.
- Use a non-soap cleanser.
- Apply cornstarch powder after bathing.
- Avoid caffeinated food and drink.
- Discontinue any drug that may be causing hyperhidrosis.
- Apply antiperspirant.
- Topical antiperspirants
Deodorants are fragrances or antiseptics to disguise unpleasant smells; on their own, they do not reduce perspiration.
Antiperspirants contain 10–25% aluminium salts to reduce sweating; “clinical strength” aluminium zirconium salts are more effective than aluminium chloride.
Topical anticholinergics such as glycopyrrolate and oxybutynin gel have been successful in reducing sweating; cloths containing Glycopyrronium tosylate (Qbrexza ) were approved by the FDA in July 2018 for axillary hyperhidrosis in adults and children 9 years of age and older. Dusting powder is available containing the anticholinergic drug, diphemanil 2%.
) were approved by the FDA in July 2018 for axillary hyperhidrosis in adults and children 9 years of age and older. Dusting powder is available containing the anticholinergic drug, diphemanil 2%.
Antiperspirants are available as a cream, aerosol spray, stick, roll-on, wipe, powder, and paint.
Specific products are available for different body sites such as underarms, other skin folds, face, hands and feet. They are best applied when the skin is dry, after a cool shower just before sleep.
- Wash off in the morning if tending to irritate.
- Use from once weekly to daily if necessary.
- If irritating, apply hydrocortisone cream short-term.
- Iontophoresis is used for hyperhidrosis of palms, soles and armpits.
- Mains and battery-powered units are available.
- The affected area is immersed in water, or, with a more significant effect, glycopyrronium solution.
- A gentle electrical current is passed across the skin surface for 10–20 minutes.
- Repeated daily for several weeks then less frequently as required
- Iontophoresis may cause discomfort, irritation or irritant contact dermatitis.
Oral anticholinergic drugs:
Available drugs are propantheline 15–30 mg up to three times daily, oxybutynin 2.5–7.5 mg daily, benztropine, and glycopyrrolate (unapproved). They can cause dry mouth, and less often, blurred vision, constipation, dizziness, palpitations and other side effects. People with glaucoma or urinary retention should not take them.
Caution in older patients: increased risk of side effects is reported, including dementia.
- Oral anticholinergics may interact with other medications.
- Beta-blockers
- Beta-blockers block the physical effects of anxiety.
- They may aggravate asthma or symptoms of peripheral vascular disease.
- Calcium channel blockers, alpha-adrenergic agonists (clonidine), nonsteroidal anti-inflammatory drugs and anxiolytics may also be useful for some patients.
- Botulinum toxin injections
- Botulinum toxin injections are approved for hyperhidrosis affecting the armpits.
- The injections reduce or stop sweating for three to six months.
- Botulinum toxins are used off-license for localized hyperhidrosis in other sites such as palms.
- Topical botulinum toxin gel is under investigation for hyperhidrosis.
- Overactive sweat glands in the armpits may be removed by several methods, usually under local anesthetic.
- Tumescent liposuction (sucking them out)
- Subcutaneous curettage (scraping them out)
- Microwave thermolysis (the MiraDry® system approved by FDA in 2011)
- High-intensity micro-focused ultrasound (experimental)
Surgery to cut out the sweat gland-bearing skin of the armpits. If a large area needs to be removed, it may be repaired using a skin graft
Sympathectomy: Division of the sympathetic spinal nerves by chemical or surgical endoscopic thoracic sympathectomy (ETS) may reduce sweating of face (T2 ganglion) or armpit and hand (T3 or T4 ganglion) but is reserved for the most severely affected individuals due to potential risks and complications.
Hyperhidrosis may recur in up to 15% of cases. Sympathectomy is often accompanied by undesirable skin warmth and dryness. New-onset hyperhidrosis of other sites occurs in 50–90% of patients and is severe in 2%. It is reported to be less frequent after T4 ganglion sympathectomy compared with T2 ganglion sympathectomy. Serious complications include Horner syndrome, pneumothorax (in up to 10%), pneumonia and persistent pain (in fewer than 2%).
Lumbar sympathectomy is not recommended for hyperhidrosis affecting the feet, as it can interfere with sexual function.
Future treatments for hyperhidrosis
Several research projects are underway to find safer and more effective treatments for hyperhidrosis. These include:
Topical anticholinergic DRM04
Combination of oxybutynin and pilocarpine (to counteract the adverse effects of the anticholinergic, oxybutynin) THVD-102
Not all cases of hyperhidrosis are preventable. For example, you can’t prevent focal hyperhidrosis since it may have a genetic cause. If you have generalized hyperhidrosis, managing or treating any underlying health conditions can help. You can also work with your healthcare provider to manage the side effects of medications you’re prescribed to reduce the likelihood of hyperhidrosis.
]]>
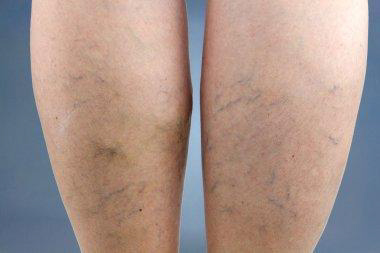
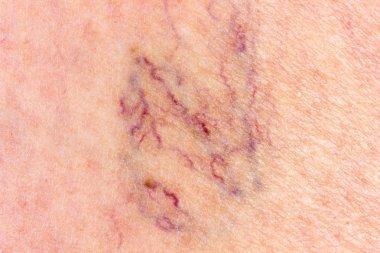
There’s usually no need to worry. Spider veins aren’t dangerous by themselves. They simply mean some small blood vessels are damaged. Spider veins are mostly a cosmetic issue, meaning you might not like their appearance, but they won’t harm you.
Spider veins are common. They affect more than 50% of women and people assigned female at birth (AFAB), and they become even more common after age 80. Spider veins are more common among women and people AFAB compared with men and people assigned male at birth
Sometimes, though, spider veins are an early sign of chronic venous insufficiency (CVI). This is a vein disease that can affect your quality of life and lead to complications.
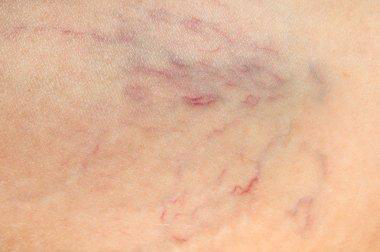
Telangiectasias need to be distinguished from other vascular conditions, including blood vessel tumors such as infantile hemangioma and angiomas that arise in adults; and capillary or venous vascular malformations.
Large red blood vessels are arteries and large blue blood vessels are veins. Arteries may be enlarged due to aneurysm formation. Veins enlarged due to the destruction of their valvular system are known as varicose veins.
Causes of spider veins:
In the legs, spider veins can occur when the valves inside the veins stop working correctly. Veins carry blood back to the heart. To prevent blood from flowing backward, they contain a one-way valve that closes once the blood passes through it.
If this valve weakens or sustains damage, the blood may have difficulty flowing in the correct direction, and it can begin to pool inside the vein. Over time, this can cause a bulge in the vein that branches out, resulting in spider veins.
Spider veins on the face are often the result of tiny blood vessels bursting. Increased pressure or sun damage can cause these to occur.
Factors that can increase a person’s risk of developing spider veins include:
- Genetics: Up to 90% of people with spider veins have a family history of them.
- Pregnancy: An increase in blood flow and the extra weight of the fetus on leg veins during pregnancy may cause spider veins.
- Sex: Spider veins occur in 41% of females ages 50 years and older. They tend to affect females almost twice as much as males.
- Age: The valves in veins tend to get weaker over time. The calf muscles, which help support the veins in the legs and enable them to pump blood upward, may also lose some of their strength as a person ages.
- Having overweight: Extra body weight can place added pressure on leg veins.
- Hormones: Hormonal birth control and hormonal treatments for menopause may increase the risk of spider veins. This is because estrogen can weaken vein valves.
- Sitting or standing for extended periods: Veins in the legs have to work harder to pump blood up toward the heart when a person remains in the same position for more than 4 hours
- Past blood clots or vein damage: This can damage the valves and make them unable to work correctly.
- Excess pressure in the face: This can be due to forceful coughing, sneezing, or vomiting. Some people may get spider veins on their face after pushing during childbirth.
- Sun damage: UV light from the sun can damage the skin and cause broken blood vessels or spider veins, especially on the face.
Certain medications may give rise to telangiectasia.
- Vasodilators especially calcium channel blockers; sun-exposed sites are mainly affected
- Long-term systemic corticosteroids
- Long-term topical corticosteroids, including steroid rosacea
- Intralesional triamcinolone injections
Telangiectasia may follow a cutaneous injury. For example:
- Scarring, including hypertrophic and keloid scars
- Livedoid vasculopathy and atrophy blanche
- Radiation damage
- Atrophie blanche
Classification:
Inherited conditions
Hereditary hemorrhagic telangiectasia: Hereditary hemorrhagic telangiectasia (HHT) is also known as Osler-Rendu-Weber syndrome. It is a rare inherited disorder that affects blood vessels throughout the body and is characterized by a tendency for bleeding in particular recurrent epistaxis (nosebleeds); and skin telangiectasia (skin lesions resulting from dilation of blood vessels).
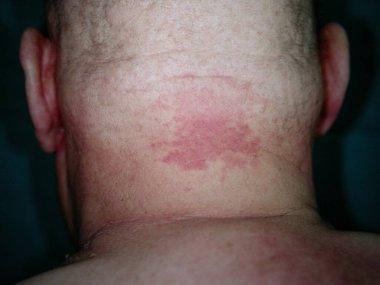
The two major types of HHT are HHT1 and HHT2. They are caused by mutations in the endoglin (ENG) and activin receptor-like kinase type 1 (ACVLR1) genes found on chromosomes 9 and 12 respectively. Two other genes have also been identified. A defect in just one of these genes causes an abnormality in the formation of blood vessels, which may easily rupture and bleed. The abnormal blood vessels are known as Telangiectasias, or arteriovenous malformations (AVM) if larger blood vessels are involved.
The diagnostic criteria for HHT are:
- Spontaneous recurrent nosebleeds
- Multiple Telangiectasias on skin and mucous membranes
- Involvement of internal organs
- An affected parent, sibling or child
Benign hereditary telangiectasia: Benign hereditary telangiectasia is a primary telangiectatic disorder. It has varying clinical patterns. They are often widely distributed over the face, neck, upper trunk, dorsal, hands and, less frequently, knees. Telangiectasias may be macular, plaque-like, arborizing, reticulated, punctate, mottled, spiderlike, and linear.
- Punctate Telangiectasias may be surrounded by pale halos (steal phenomenon).
- Some lesions may be indistinguishable from spider telangiectasis.
- Early Telangiectasias can be small and erythematous. They often increase in size and may become paler with age.
- The mucosal membranes are not affected with the exception of the vermilion border of the lips.
- There is no systemic involvement or bleeding, in contrast to hereditary hemorrhagic telangiectasia.
- The Telangiectasias are invariably asymptomatic and cause only mild cosmetic concerns.
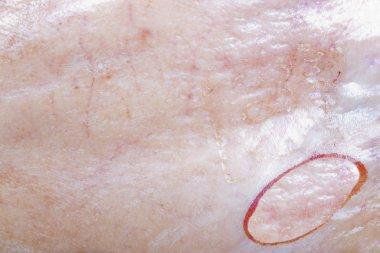
Generalized essential telangiectasia:
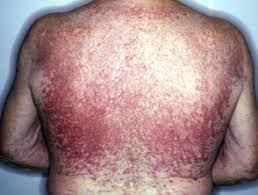
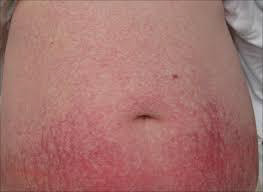
Generalized essential telangiectasia is just one type of primary telangiectasia and is given this name because of its widespread distribution pattern over the body. The cause of generalized essential telangiectasia remains unclear. Sometimes there may be a family history, which suggests a genetic component.
Unilateral nevoid telangiectasia: Unilateral nevoid telangiectasia is a rare congenital or acquired disorder. The majority of the authors propose that it is probably related to elevated estrogen receptors, although other authors advocate different theories.
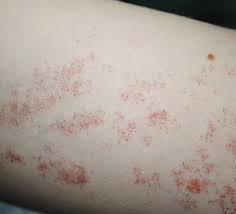
Angioma serpiginous: Angioma serpiginous is a skin condition in which there are small blood vessels near the skin surface. It presents as small red dots (puncta) that cluster together to form a linear or snake-like array (serpiginous pattern) or ring-shaped (gyrate) pattern. There is no bleeding, inflammation or pigmentation.
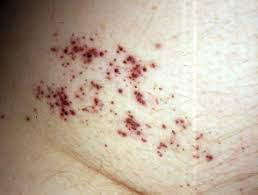
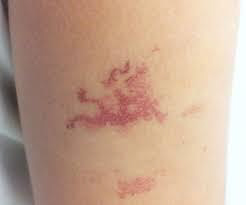
Rothmund Thompson syndrome: Rothmund–Thomson syndrome is a rare inherited disease that affects the skin, eyes, bones, and internal organs. At least 300 cases have been reported in medical journals since a case was first described by Rothmund in 1868. Rothmund–Thomson syndrome is also known as poikiloderma congenitale.
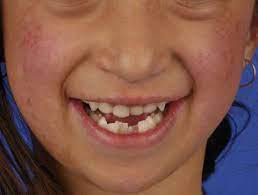
Rothmund–Thomson syndrome is due to a genetic defect, in which there are mutations in the RECQL4 gene on Chromosome 8. This gene encodes for the enzyme DNA helicase which unwinds DNA (deoxyribonucleic acid). The abnormal gene makes the chromosomes unstable, altering the growth of cells in many tissues.
Ataxia-telangiectasia:
Ataxia-telangiectasia is a rare inherited multisystem disorder that is characterized by:
- Ataxia (lack of co-ordination)
- Telangiectasias on the skin and eyes
- Severe combined immunodeficiency resulting in recurrent respiratory infections
- A predisposition to malignancy.
- Ataxia-telangiectasia is also known as Louis-Bar syndrome.
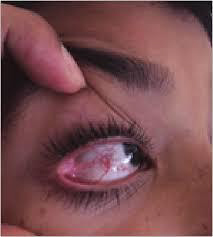
Ataxia-telangiectasia may occur in any race or sex. Reported rates of incidence range from 1 in 40,000 to 1 in 100,000 births. The incidence of ataxia-telangiectasia is significantly higher when parents are consanguineous, for example in the Bedouin population.
Bloom syndrome (congenital telangiectatic erythema): Bloom syndrome is an autosomal recessive inherited disorder, which means that two abnormal Bloom syndrome genes are needed for the disease to be apparent (one from each parent). If a person has one affected gene, he or she is called a carrier of Bloom Syndrome and does not manifest symptoms of the disease. If both parents are carriers, there is a 1 in 4 chance of having an affected child with each pregnancy. Recessive diseases are often consanguineous (eg, cousin marriages).
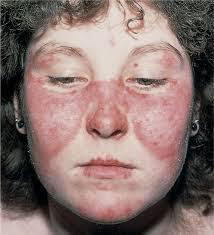
Bloom syndrome is more common in eastern European Ashkenazi Jews. At least 1 in 100 Ashkenazi Jews is a carrier of the disease. It appears to be slightly more common in males than females.
Cockayne syndrome:
Cockayne syndrome is a rare inherited disorder in which people are sensitive to sunlight, have short stature, and have the appearance of premature aging. In the classical form of Cockayne syndrome (Type I), the symptoms are progressive and typically become apparent after the age of 1 year.
Cutis marmorata telangiectasia congenita:
Cutis marmorata is a condition where the skin has a pinkish blue mottled or marbled appearance when subjected to cold temperatures. Rewarming usually restores the skin to its normal appearance. Cutis marmorata occurs in about 50% of children and is typically seen throughout infancy. Adults may also be affected.
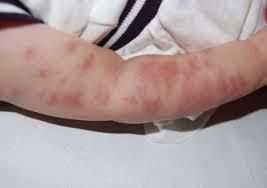
The mottled appearance of cutis marmorata is caused by superficial small blood vessels in the skin dilating and contracting at the same time. Dilation creates the red color of the skin whilst contraction produces a pale appearance. This phenomenon is most pronounced when the skin is cooled. The reasons for the reaction are not fully understood.
Focal dermal hypoplasia (Goltz syndrome):
Focal dermal hypoplasia is a genetically inherited disorder that can affect the development of many different organ systems and was first described by Goltz in 1962. It presents with characteristic abnormalities of the skin, eyes and teeth and may also have effects on the skeletal, gastrointestinal, genitourinary, neurological and cardiovascular systems. The name is actually misleading, as thinning of tissues is not confined to the dermis but also involves the epidermis and subcutaneous tissue.
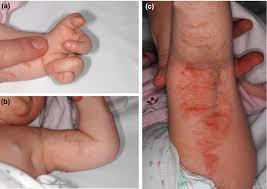
Kindler syndrome:
Kindler syndrome is a rare hereditary disorder, associated with skin fragility. The syndrome involves the skin and mucous membrane with radiological changes. The genetic defect has been identified on the short arm of chromosome 20.
Acquired telangiectasia
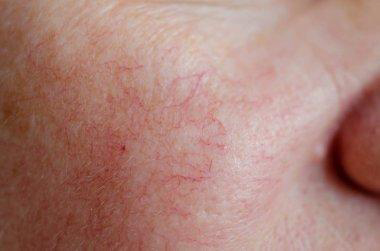
Rosacea: Rosacea is a chronic inflammatory skin condition predominantly affecting the central face and most often starts between the age of 30–60 years. Rosacea typically presents after the age of 30 and becomes more prevalent with age. However, it can occur at any age and occasionally presents in children. Although rosacea can affect anyone, it is more common in those with fair skin, blue eyes, and those of Celtic or North European descent. It may be more difficult and under-recognized in patients with skin of color.
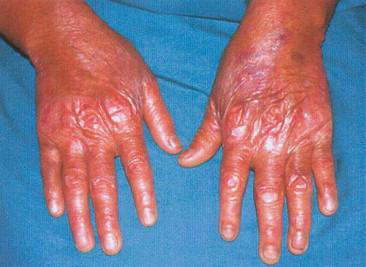
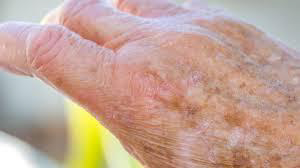
Sun damaged and aged skin especially in those who smoke:
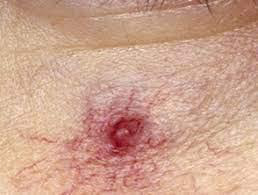
Spider telangiectasis (also called spider naevus): A spider telangiectasis is composed of dilated blood vessels, and is clinically characterized by its spider-like appearance. It is given that name because it has a central red papule (the body of the ‘spider’) from which fine red lines (the spider legs) extend radially. An alternative explanation for the name explains that the red lines form a spider-like network. Other names for spider telangiectasis are spider angioma (a misnomer), spider naevus and naevus araneus.
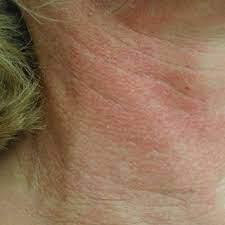
Poikiloderma of Civatte (sun damage affecting the sides of the neck): Poikiloderma of Civatte is a benign, common and chronic condition, which belongs to the group of melanodermas (pigmented skin disorders). The term ‘poikiloderma’ refers to a skin change with atrophy where hypopigmentation/hyperpigmentation changes and dilation of the fine blood vessels (telangiectasia) can be seen in the affected skin. Long-term sun exposure is considered to be a main contributing factor.
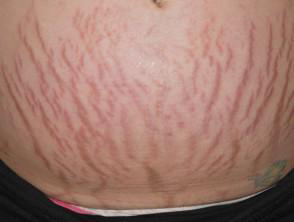
Pregnancy:
During pregnancy there are marked changes in sex hormones, the immune system, and the cardiovascular system, and this can lead to changes in the skin. Many changes in the skin, hair, and nails of pregnant women are common and considered normal (physiological).
Pigmentation in pregnancy
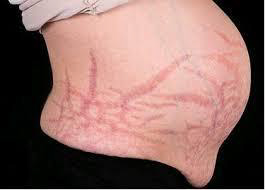
Linea nigra, darkening of pigmented areas (ie, nipples, areolae, genitals), and generalized increase in pigmentation appears in the first trimester of pregnancy. It affects 90% of pregnant women, particularly those with skin of color (Fitzpatrick skin types IV-VI). This pigmentation fades after delivery, but usually not completely.
Cushing syndrome: Cushing syndrome is a hormonal disorder caused by prolonged exposure to inappropriately high levels of plasma glucocorticoid (also referred to as cortisol) hormones. Glucocorticoid hormones maintain glucose regulation, suppress the immune response and are released as part of the body’s response to stress. The production of cortisol from within the cortex of the adrenal glands is regulated by a small gland just below the brain called the pituitary gland.
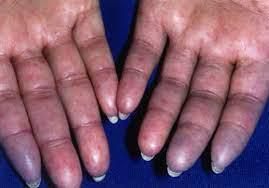
Systemic sclerosis especially CRST syndrome (which forms telangiectatic mats): Systemic sclerosis (SSc) is an autoimmune inflammatory condition. It results in potentially widespread fibrosis and vascular abnormalities, which can affect the skin, lungs, gastrointestinal tract, heart and kidneys. The skin becomes thickened and hard (sclerotic).
Cutaneous lupus erythematosus: Cutaneous lupus erythematosus (LE) is a diverse group of autoimmune connective tissue disorders localized to the skin that can be associated with systemic lupus erythematosus (SLE) to varying degrees.
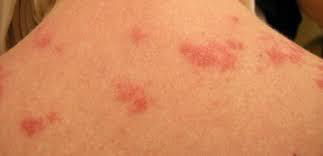
Cutaneous lupus erythematosus has an annual incidence of 4 cases per 100,000 people, and a prevalence of 73 cases per 100,000.
As with SLE, there is a marked female predominance with CLE particularly affecting women 20 to 50 years of age. However, all age groups and both sexes can be affected. Skin of color is an important predisposing factor.
Mixed connective tissue disease: Mixed connective tissue disease is a rare autoimmune connective tissue disorder with anti-U1RNP auto-antibodies. The cause of mixed connective tissue disease is not fully known. Due to the presence of autoantibodies, it is classified is an autoimmune disease. It is most common in patients with HLA-DR4, suggesting it has a genetic background.
Dermatomyositis: Dermatomyositis is a rare disease that causes muscle weakness and skin rash. Symptoms include a red or purple rash on sun-exposed skin and eyelids, calcium deposits under the skin, muscle weakness, and trouble talking or swallowing. There is no cure, but treatment is done to reduce the symptoms.
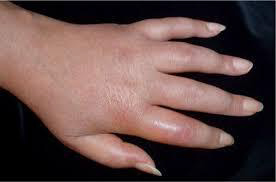
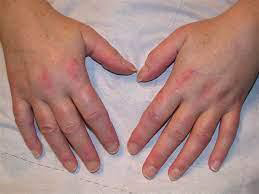
Mastocytosis, specifically the variant, Telangiectasia macularis eruptiva perstans: Mastocytosis is a diverse group of disorders characterized by the expansion and accumulation of mast cells in one or more organ systems. It can affect the skin, bone marrow, liver, spleen, gastrointestinal tract, or lymph nodes. In 2022, the World Health Organisation (WHO) categorized three main types of mastocytosis:
- Cutaneous mastocytosis (affecting the skin alone), most commonly maculopapular cutaneous mastocytosis
- Systemic mastocytosis
- Mast cell sarcomas
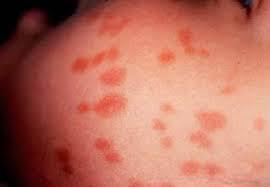
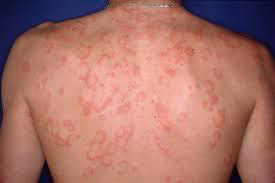
Mastocytosis can occur at any age, although some types are more common in particular age groups. Females have a slightly higher risk of developing mastocytosis than males. In most cases, there is no family history of mastocytosis.
Carcinoid syndrome:
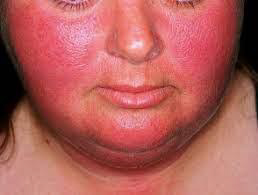
Carcinoid syndrome is characterized by episodic cutaneous flushing, diarrhea, and wheezing. Carcinoid syndrome is the result of a combination of peptides and amines secreted by advanced neuroendocrine tumors (NETs) into the bloodstream. Carcinoid syndrome affects up to 19% of people with neuroendocrine tumors, which can be present in the gut, pancreas, lung, kidney, ovaries, and testes. They are rare in children. The incidence is 1–2 per 100,000 people annually.
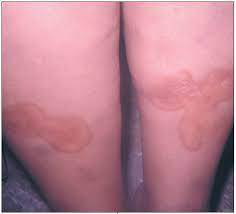
Necrobiosis lipoidica: Necrobiosis lipoidica is a rare granulomatous skin disorder typically described on the shin of diabetics. Necrobiosis lipoidica is three times more common in females than in males, and usually develops in young and middle-aged adults. Necrobiosis lipoidica begins as a dull red papule or plaque on the shin which slowly enlarges into one or more yellowish-brown patches with a red rim.
Male genital dysaesthesia:
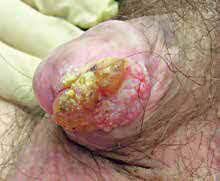
Male genital dysaesthesia is a form of cutaneous dysaesthesia characterized by a burning, hot, irritating discomfort of the penis, foreskin, and/or scrotum. It is often accompanied by increased sensitivity to touch.
Male genital dysaesthesia is also known as Dysaesthetic penoscrotodynia (DPSD) or male genital burning syndrome. If dysaesthesia is accompanied by redness, this may be referred to as red scrotum syndrome. Localized symptoms can be described as scrotodynia or burning scrotum syndrome.
Male genital dysaesthesia can affect males of all ages and skin color. It is more common amongst those with Fitzpatrick type 1 or 2 skin, and those over the age of 50. Genital dysaesthesia associated with redness and vascular hyperreactivity of the scrotum may be associated with rosacea.
Treatment
There are different treatment options a person can try:
- Compression stockings or socks
- Wearing compression stockings or socks places pressure on the veins in the lower legs. This pressure can help improve blood flow and prevent further spider or varicose veins.
- Compression stockings may also help relieve leg swelling and lower the risk of blood clots in the legs.
Types of compression stockings include:
- Support pantyhose: These provide only light pressure but are available in many stores.
- Gradient compression stockings and socks: These provide medium pressure around the feet, ankles, and calves. They are often available at specialist stores and pharmacies.
- Prescription compression stockings: These provide the most pressure to the feet and legs. They come in various sizes and strengths, as well as footless varieties. Prescription compression stockings are not suitable for some people, including those who have heart failure or other heart problems.
- Sclerotherapy and closure system: Sclerotherapy involves injecting an irritant directly into the affected vein. Due to irritation, the veins stick together and keep blood from flowing into the area. This procedure can reduce swelling and cause the vein to shrink. Over time, the spider vein fades or vanishes. Several treatments may be necessary to obtain the desired result.Similar to sclerotherapy, closure system treatment involves injecting a substance into the affected veins. This substance is sticky, and it closes the vein off from blood flow, causing the spider vein to fade or disappear with time.As with sclerotherapy, a person may require several treatments to produce the desired outcome.
- Laser treatment: A healthcare professional can use a laser to treat small spider veins close to the skin’s surface. The laser is a strong, focused beam of light that causes the spider vein to clot and dry up.Laser treatments are less invasive than sclerotherapy and closure systems because there is no injection. However, laser treatments are typically less effective in reducing spider veins.
- Endovenous laser therapy (EVLT): EVLT is a newer procedure for treating spider veins and small varicose veins. Endovenous means that the procedure is done inside the vein.A healthcare professional makes a small incision in the affected vein and then inserts a laser fiber. The laser applies heat directly to the vein and causes it to collapse. The vein may take several months or up to a year to disappear. EVLT involves the use of local anesthesia.
- Surgery: Although some surgical treatments can be effective for larger varicose veins, doctors typically do not perform them on spider veins.
Prevention
Certain lifestyle changes and self-care tips can help prevent new spider veins from appearing or stop existing ones from getting worse. These include:
- Wearing sunscreen: Applying sunscreen every day can help prevent spider veins, particularly on the face. Use sun-protective hats and clothing when outdoors for extended periods.
- Reaching or maintaining a moderate weight: This helps reduce pressure on the veins and keeps blood flowing well.
- Wearing compression stockings: If spider veins or varicose veins are a concern or run in the family, consider wearing compression stockings or socks.
- Staying mobile: Avoid sitting or standing for extended periods without taking a break.
- Avoiding tight clothing: Clothing that is too tight around the waist, legs, or pelvis can restrict blood flow and may increase the risk of spider veins.
- Avoiding overuse of hot tubs and saunas: Excessive heat can cause veins to swell, increasing the risk of dilated and bulging veins in the legs.
- Limiting alcohol consumption: Drinking alcohol can cause flushing in the face and broken blood vessels in some people.
- Getting regular exercise: Physical activity can help improve circulation and prevent blood from pooling in the legs.
- Elevating the legs: Raising the legs when sitting or lying down can help prevent blood from pooling downward in the legs.
- Contacting a dermatologist: People with skin conditions that can increase the risk of spider veins, such as rosacea, may want to consider contacting a doctor or dermatologist to discuss treatment options.
- Using cover-up products: If the appearance of spider veins is a concern, people may wish to use body or leg makeup to mask or minimize them temporarily. Self-tanning products can also work for this purpose.